JTECH BLOG



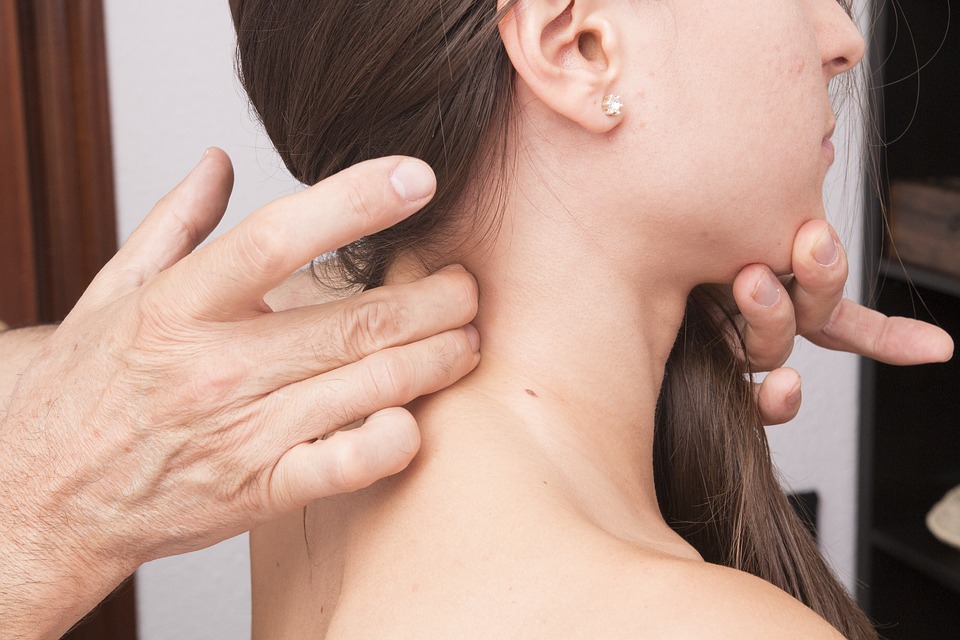
4 Tips To Reduce Muscle Pain
With over 650 muscles in the human body, it's no surprise that many people suffer from regular muscle pain and stiffness. Even with people having different pain thresholds, everyone experiences muscle pain at some point, whether as the result of an injury, a chronic condition, or just overuse. Here are a few tips you can use to avoid muscle pain and discomfort on a regular basis.
Stretch Often
For some people, muscle stiffness and pain is the result of not properly stretching on a regular basis. Stretching and gentle exercise can help strengthen muscles, preventing additional pain and stiffness. Don't push yourself too far when stretching, though, or you could hurt your muscles instead of helping them.
Exercise Carefully
If your muscle soreness is the result of an injury, be careful not to worsen the injury when exercising or staying active. Give yourself time to recover from an injury before exercising again, and start slow to avoid worsening an injury. Some muscle pain can be the result of overuse; in these cases, it might be time to change up your exercise routine to give your sore muscles a break.
Fix Your Posture
Have you noticed your back or shoulders getting sore after a long day at the office? It could be the result of poor posture. Having poor posture could affect the muscles in your back and neck after a while. If you catch yourself slouching, try to sit up straighter; it could help alleviate some pain. Take breaks throughout the day if your job has you sitting at a desk most of the time. This will help you remember to readjust and be mindful of your posture.
Use Physical Therapy Tools
Certain types of rehab tools and systems can be used in relieving muscle pain. Chiropractic alignment tools are often used to help with back pain and muscle pain. If your pain is becoming chronic, talk to your medical professional about using chiropractic alignment tools.
Having the right tools and equipment to address your muscle pain and soreness could help alleviate some discomfort. For more information on rehabilitation devices and software, contact JTECH Medical today.
Share this article:

Get a Grip! What Does My Grip Strength Reveal About My Health?
While you might think that your grip strength is only good for a firm handshake, the strength of your hands can actually be a predictive indicator of your overall health. As such, many chiropractors and doctors will use physical therapy equipment designed to test your grip among other automatic strength tests.
But what does your grip strength say about your overall health? Here are some of the primary indicators about your health that doctors, chiropractors, and more can glean from a simple grip test.
But first: What is grip strength?
Before we dive into the importance of grip strength, we need to know what it is and how it's measured.
Grip strength is synonymous with hand strength and it is a measure of the muscle health of your hands and forearms. Grip strength is typically measured in pounds, kilograms, or Newtons by squeezing a type of muscle strength testing equipment, known as a dynamometer, about three times in each hand. The average healthy grip strength for men is a squeeze of about 72.6 pounds while women typically measure around 44 pounds.
Should your score fall below this measurement, it could be an indicator of a variety of health issues. Keep in mind that grip strength often decreases as you grow older and it isn't a measurement of your pain thresholds. Here are some of the many ways grip strength can reveal hidden issues in your health.
Physical therapy
Grip strength is often a good measurement of how physical therapy is going for an injured patient. Because sensitive pieces of physical therapy equipment are used to track even the slightest changes in grip strength, this can be a good indicator for tracking the progress of physical therapy patients. A stronger grip will imply that someone is benefiting from the physical therapy while a weaker grip suggests a change in therapy is necessary.
Cardiovascular health
Your grip strength can also indicate the strength of your heart health. According to the Harvard Medical School, a decrease in grip strength of about 11 pounds is linked to a 17% increased risk for heart disease and dying from it as a result. It's also linked to a 7% increased risk for heart attack.
Even when researchers attempted to adjust their study of more than 140,000 adults for external factors, including smoking and age, they still found that grip strength was a stronger indicator for cardiovascular disease than blood pressure. Grip strength can also indicate your risk for stroke and serve as a reliable measurement of your biological age, not your chronological age.
How can I improve my grip strength?
You can improve your grip strength by engaging in a variety of hand exercises. This can be as simple as lifting weights or using a shovel to improve your home's garden. You can also talk to your doctor; they have a variety of rehab tools and systems which work to improve your overall health. Since grip strength tends to increase when you better your overall health, engaging in other forms of physical therapy and exercise is encouraged. In fact, just 10 minutes of exercise or other physical activity every day can help you improve your mobility, avoid disability, and live even longer.
Your grip strength and range of motion are valuable indicators of your overall health. Rely on a doctor who uses functional assessment tools and a range of physical therapy equipment when you want to take your strength into your own hands...err, grip. Contact JTech Medical today for more information on physical therapy equipment.
Share this article:
9 Reasons to Check Out a Chiropractic Clinic

If you are suffering from health problems such as headaches, back pain, or plain old stress, going to a chiropractor may be the best thing you can do. They use back adjustment tools and techniques that can do a lot more than put your spine back into alignment. In fact, many chronic pain conditions can be helped by a visit to your local chiropractor. Here are some of the health benefits of getting Chiropractic care:
- Getting regular treatments can help your blood pressure. When a specialist uses a chiropractic adjusting instrument on you, it can have a profound impact on your blood pressure. This is true if yours is too low or too high. New research from the Human Journal of Hypertension shows that this kind of treatment can be as effective as some of the high blood pressure medications on the market today.
- Chiropractic adjustment tools can help with inflammation. One of the main causes of pain is swelling (inflammation). When people suffer from chronic inflammation the result can be chronic pain, cancer, and heart disease. At least 350 million people around the globe suffer from this. Chiropractic treatment can reduce inflammation.
- Chiropractors are great at helping people with neck and back pain. These are some of the main problems that prompt people to seek out care from a chiropractic office. Back pain is very common around the world. It has been estimated that about 80% of people in the United States will suffer from back pain of one kind or another some time during their lives. When a back adjustment tool or technique is used, the results can be the immediate alleviation of back or neck pain.
- Adjustments can straighten out the spine. Many people suffer from scoliosis. This is when the spine is curved in an abnormal way. There are not a lot of things that can be done to correct this problem. Getting chiropractic adjustments can help. When used with physical therapy, scoliosis can be treated and the general progression can be halted.
- It can help with leg pain. The sciatic nerve goes down the back of both legs. Often when there a problem with a disc in the back, pain can radiate down these nerves. This is referred to as "sciatica" and can be very painful. A lot of people turn to medications to help with this kind of discomfort or pain but that has its own limitations. When a chiropractic alignment tools are used on people with sciatic pain, they usually find at least some relief.
- These treatments can help people who suffer from headaches. There are a number of different kinds of headaches and therefore a number of causes. Migraines and tension headaches are some of the most severe and are usually the result of spinal issues or a painful back. When the spine is not aligned correctly, it can cause tension in the muscles and that can cause headaches. After back and neck pain, headaches are the most common problem that brings people into chiropractic clinics.
- A chiropractor can help with neurological problems. Using back adjustment tools and techniques can lead to an increase in the amount of cerebral fluid and blood that gets to the brain. People who suffer from conditions such as epilepsy and multiple sclerosis can be really helped. This area is still being researched but so far it shows promise for people with these and other neurological problems.
- A chiropractor can help you be better at your sport. When people are trying to improve the way they play sports, getting into good shape is a natural thing to do. Pain and inflammation can make that a hard thing to accomplish. Because chiropractic treatments can decrease pain and swelling, it helps people stay active and perform better.
- It can help with symptoms of vertigo. When people suffer from vertigo, normal tasks can make them feel dizzy and nauseated. This is a common side effect of some neck and head injuries. While it may seem simple, this can be debilitating for the people who experience it. Back adjustment tools and techniques do a lot to reduce vertigo.
Seeing a good chiropractor can do a lot to get and keep you healthy and happy.
Share this article:
How Muscle Testing Devices Can Predict Overall Health

In a variety of industries, it's important to have reliable indicators of an individual’s overall health. This includes hospitals, obviously, but this can extend far beyond that as well: insurance, pain management clinics, therapy, and more. Manual muscle testing devices can be an excellent predictor of overall health. Here's how these physical therapy tools can be used to indicate a person's health.
Muscle Strength
Manual muscle testing devices allow users to assess how someone is recovering from an illness or injury impairing or affecting their overall muscle strength. This type of muscle strength testing equipment can help professionals determine if existing treatments have been working to improve a person's strength, showing progress over time. Additionally, these rehab tools can be used to assess a patient's starting point in terms of their physical strength, showing damage that may have been done during an injury, and can help identify injuries that could go unchecked. This can help in worker's compensation, physical therapy, and a variety of other fields.
Motor Control
Additionally, testing a patient with manual muscle testing devices can help assess the degree to which an injury or illness has impacted their fine motor control. Injuries involving the wrist or hand can have a potentially severe impact on the person's ability to perform fine motor skills related tasks. The human body has more than 650 muscles, and damaging even one of the muscles or tendons relating to a person's grip can limit what small motor skills they're capable of. Testing muscle strength in the hand can help determine how a person has been injured. Additionally, this sort of testing can be used in cases where motor control is limited by neurological conditions, giving a better sense of what a person's overall neurological health state might be. This can be useful in a variety of rehab settings, physical therapy, and even insurance.
Manual muscle testing machines can be incredibly useful in a variety of industries that need accurate measurements of a person's overall health and wellbeing. Muscle strength and motor control are both very useful metrics for assessing a person's health, and these devices can help measure these things accurately. For more information on these useful rehabilitation tools and measuring devices, contact JTECH Medical Industries today.
Share this article:
The Future of America’s Opioid Epidemic
Due to the continued mishandling of opioids, the accessibility of the drug is becoming more and more regulated. As a society, we must cope with this epidemic without sacrificing the very people who need this drug to endure horrible, physical pain.
Overview of Opioids
Opioids are a broad class of drugs that include both legal and illicit substances. Examples of opioids include prescribed painkillers (such as morphine, methadone, and hydrocodone) and heroin. Common brand names that fall under this category are OxyContin, Percocet, Vicodin, and Demerol.
Opioids chemically react with opioid receptors, which are located in the nervous system as well as the brain, and release endorphins. These neurotransmitters contribute to a patient’s feelings of euphoria as well as pain relief, which often leads to its misuse. Over time, the body acclimates to the opioids and slows the release of endorphins, which leads some to increase their dosages to maintain pain relief and an altered brain state. Regular use of this drug, unfortunately, does lead to dependence—which is evident in America’s growing opioid epidemic.
America’s Opioid Epidemic

Tracing the current crisis back to one source is impossible, but there are vital pieces throughout history that we can link to this evolving puzzle. In the 1980s, the accessibility of opioids changed drastically. A drug that once was only prescribed for patients with a terminal illness, was later extended to include chronic pain sufferers. This led to a steady expansion of opioid use, propelled by an insistence that opioids were a legitimate mechanism for pain control. Researchers on the drug had also severely underestimated its addictive potential. Prescribing practices slowly began to shift as physicians issued prescriptions for larger doses in an attempt to limit refill requests and help patients better manage pain. This increased the risk of dependence for opioid users—as much as 80% of opioid abusers had a prescription for the drugs before the start of their addiction.
However, efforts to reduce opioid dependence have proved valuable. In 2006, healthcare providers wrote an average of 72.4 opioid prescriptions per 100 persons, which decreased to 58.5 prescriptions per 100 persons in 2017. This represents a reduction of over 19%, and the figures for high dosage prescriptions are similar—decreasing from 11.5 prescriptions to 5.0 prescriptions per 100 people in that same time period. The CDC Drug overdose report has concluded that opioid prescribing practices have continued to improve in recent years; yet, levels of opioid abuse and overdose continue to steadily rise.
In 2016, there was a rapid increase in opioid-related overdoses, ending in 63,632 deaths for the year. Of these, prescription opioids were responsible for 17,087 deaths. As doctors begin to restrict the access of opioids, those who start their addiction using prescription drugs turn to illegal means in order to maintain their addiction. Some patients .even transition to more potent illegal substances, like heroin.
Limits on Opioid Prescriptions
Today, doctors better understand the addictive quality of opioids and are often reluctant to increase dosages at the risk of a patient’s long-term health. At local, state, and federal levels, officials are taking measures to mitigate the overuse of opioids. There’s been an increase in the collection of public health data regarding opioid use, improved access to treatment and recovery services, as well as inventive and non-addictive methods to manage chronic pain. However, in addition to these dynamic and necessary solutions, more and more states are implementing severe controls over opioids to subdue the seemingly endless tide of overdoses and abuse.
In addressing the threat of opioids, these initiatives unfairly restrict access to pain medication by patients who demonstrate an exigent need for them, such as cancer patients and the terminally ill. In 2016, the CDC issued guidelines that opioids for treating acute pain should be issued for periods from 3-7 days. Though merely guidelines, many states adopted these standards as legal injunctions, limiting prescriptions to supplies only lasting 7 days. These limits adversely and unnecessarily constrain pain management and create further barriers for patients seeking legitimate means to address their physical suffering. Prescription-limit laws rarely exempt cancer survivors from these constraints. In fact, from 2016-2018, their usage of opioids dropped from 24% to 10%, even though many cancer survivors endure severe, lifelong pain.
Dr. Julian Grove is a pain doctor in Arizona who has worked with the state to alter prescription regulations. According to him, the effect of these laws on doctors is that "a lot of practitioners are reducing opioid medications, not from a clinical perspective, but more from a legal and regulatory perspective for fear of investigation.” Doctors are facing extreme pressures to curtail opioid prescriptions, and this hypervigilance, unfortunately, hampers the quality of life and standard of care for many patients.
More research suggests that these laws may actually be having the opposite rather than the intended effect. To cope with the possibility of patients running out of pain medication after surgery, doctors are prescribing more medicine up-front. A study performed by Dr. Jennifer Waljee reported there was an average of a 7-tablet-per-patient rise in hydrocodone prescriptions after the regulation change.
The Future of Opioid Access
Surely, the goals of pain management should be mediated with the sobering realities of opioid exploitation. One of the ways the medical community is approaching a resolution is with a $40.4 million research program to develop a more rigorous understanding behind the causes of chronic pain, susceptibility, and new avenues for treatment. In addition to further research, doctors are looking to nonopioid medication to treat post-operative pain including acetaminophen, ketorolac, and ketamine.
Ensuring sufferers have access to modern medical advancements is of the utmost importance. Pain assessment software such as JTECH’s pain management Testing Systems allow medical practitioners to properly assess a patient’s pain levels and compile data reports of the results. This technology could be instrumental in the future of opioid access and treatment of pain. The pressure algometer measures the pressure pain threshold of specific muscle locations, providing doctors with objective data to better be able to treat chronic pain. These tools also function as monitoring systems to track a patient’s progress and determine if physical therapy is a viable treatment. This technology eliminates subjectivity in diagnoses by equipping doctors with unbiased data in order to demonstrate a patient’s need for pain medication.
There are no simple solutions to a problem as complex as America’s opioid epidemic. But, with our expanding knowledge about addiction and pain, we continue to strive for superior remedies that address the needs of all Americans.
Share this article: