Latest Blog
Check out our blogs to get business tips, industry trends, and interesting facts. Read our latest posts or select from the list of topics to find the blogs of most interest to you!
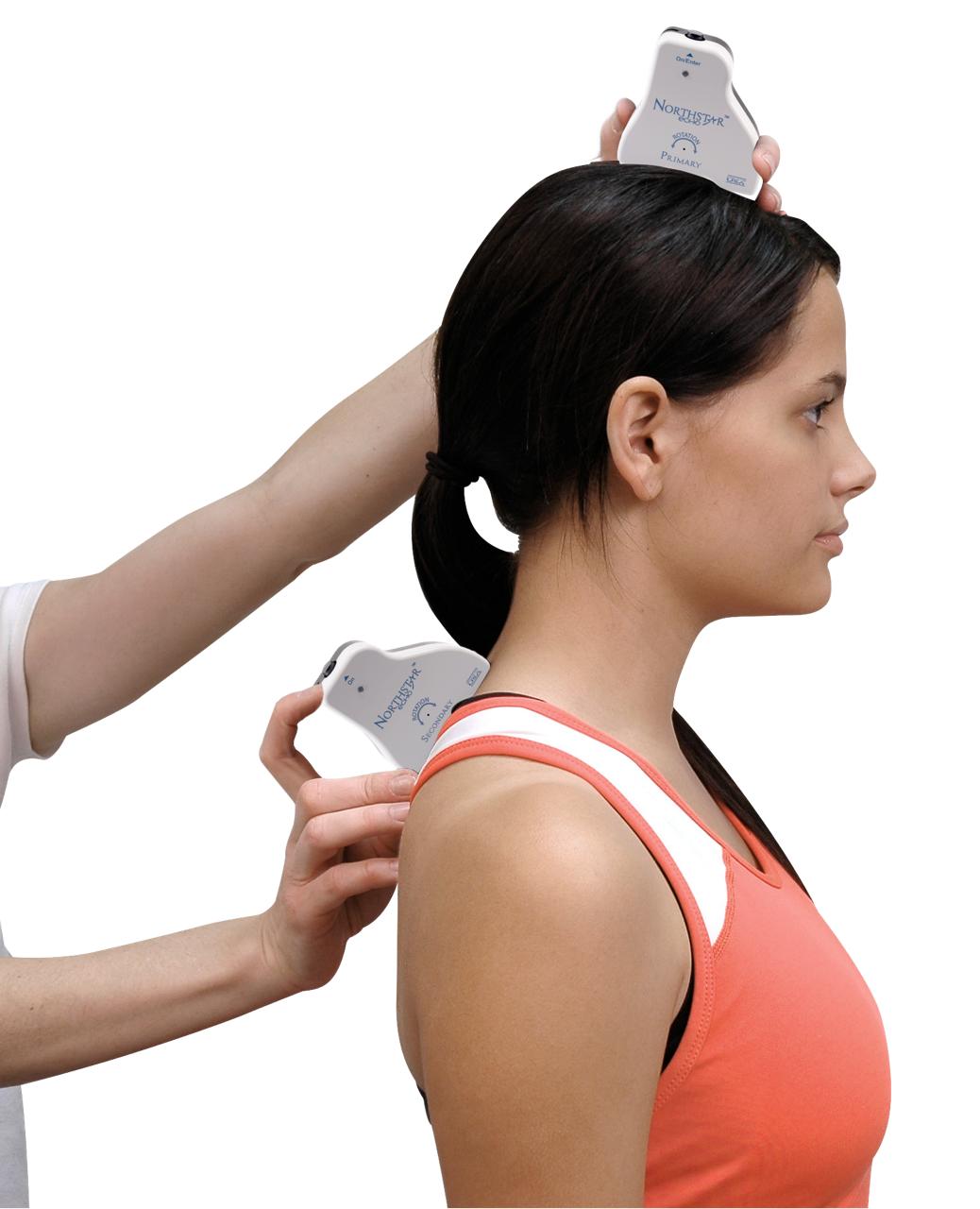
latest Post

- June 10, 2026
CPT 97750 & 95851: What Objective Testing Codes Pay in 2026
A practical guide to billing objective physical testing under CPT 97750 and 95851 in 2026 -- documentation rules, same-day bundling…

- June 09, 2026
Work Conditioning vs Work Hardening: How Occupational Medicine Clinics Choose the Right Program
A practical guide for occupational medicine clinics on choosing between work conditioning and work hardening, with CPT 97545/97546 documentation requirements…
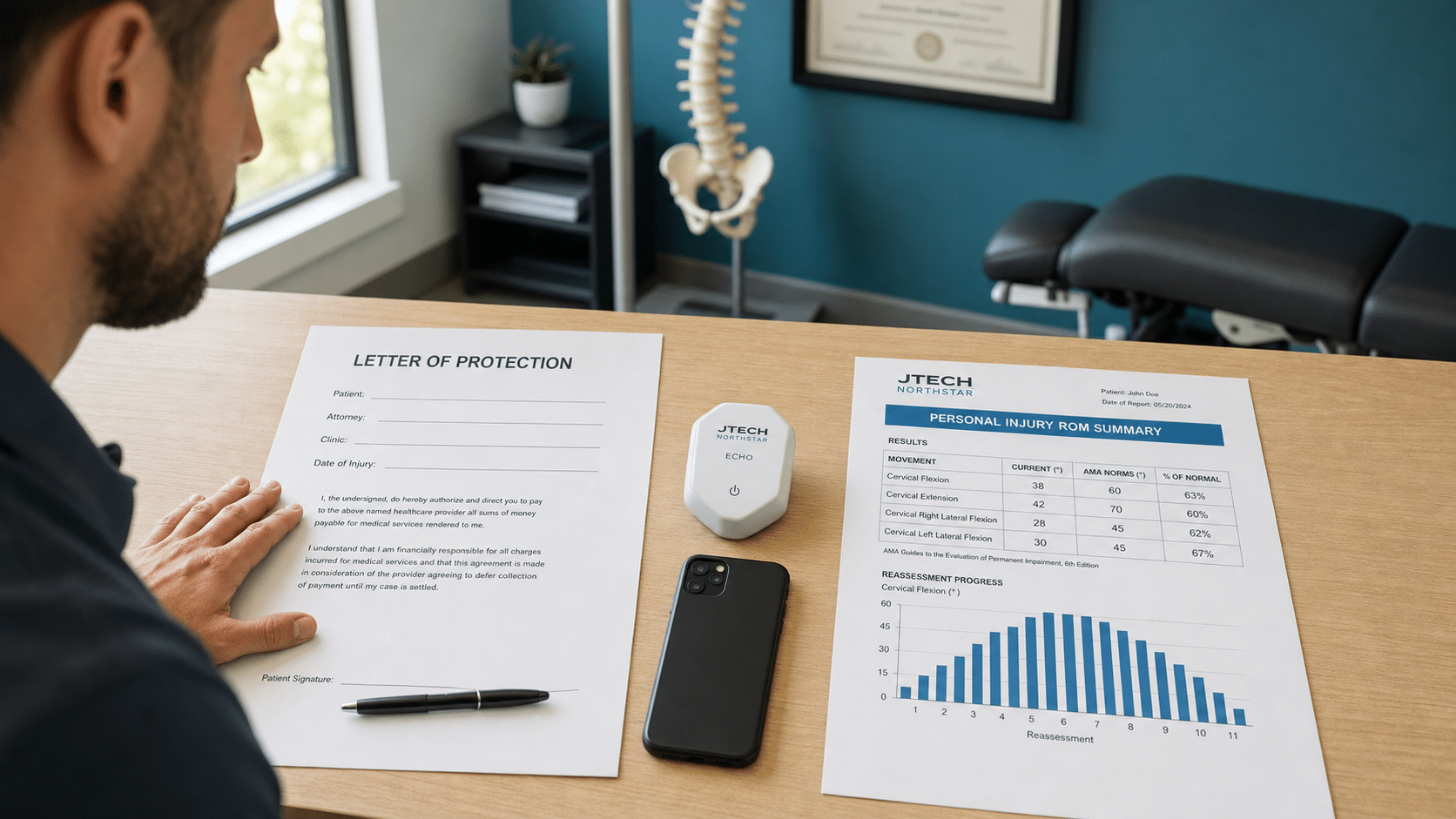
- June 05, 2026
The Personal Injury Clinic’s Letter of Protection Workflow: How to Get Your Bill Paid at Settlement
A practical letter of protection workflow for personal injury clinics: how to structure intake, document each visit, and build the…
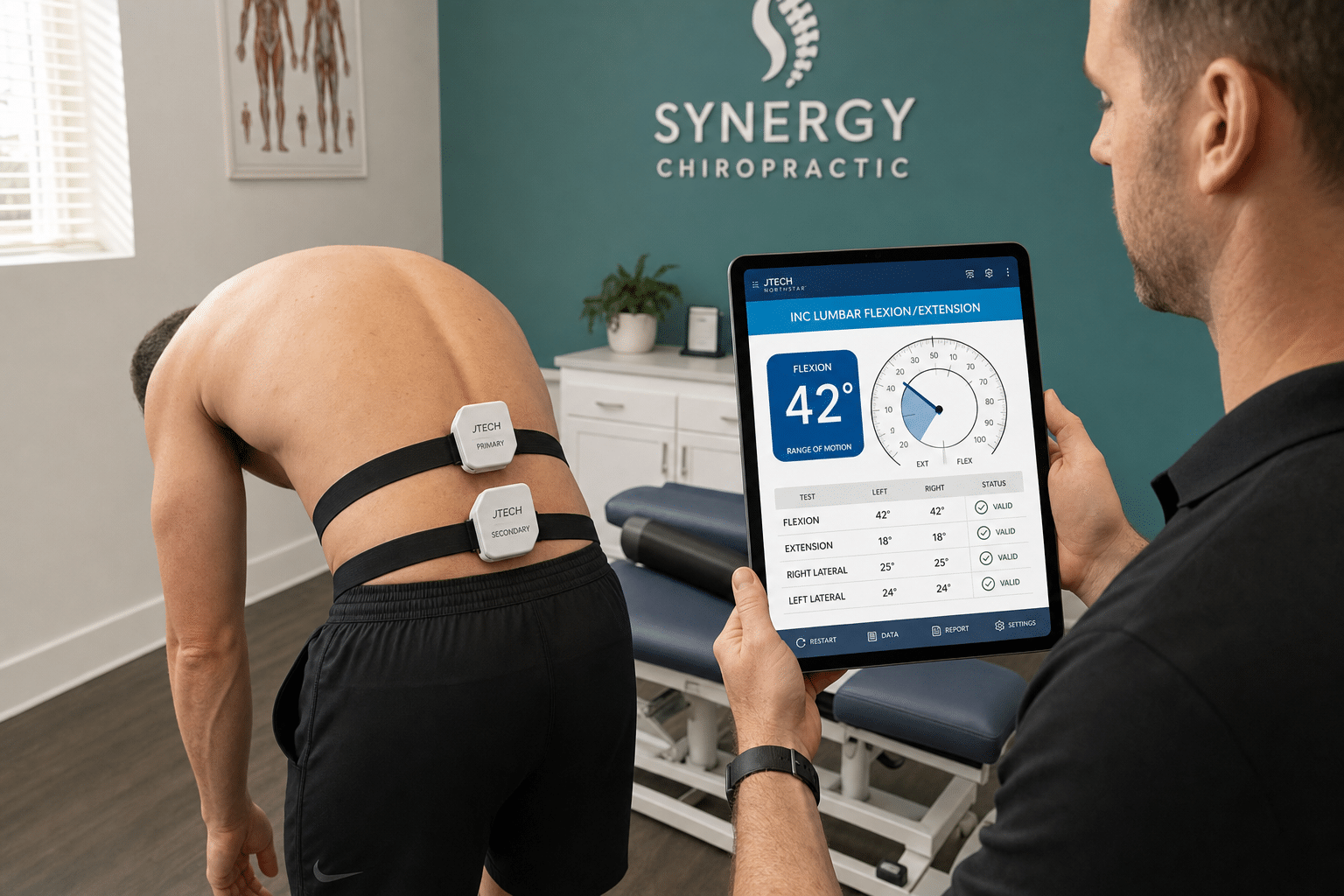
- June 03, 2026
The Chiropractor’s Lumbar Disc Workflow: A Five-Test Battery That Beats an MRI Referral
A practical lumbar disc assessment workflow for chiropractors: the five-test orthopedic battery, McKenzie directional-preference exam, and dual-inclinometer ROM baseline that…
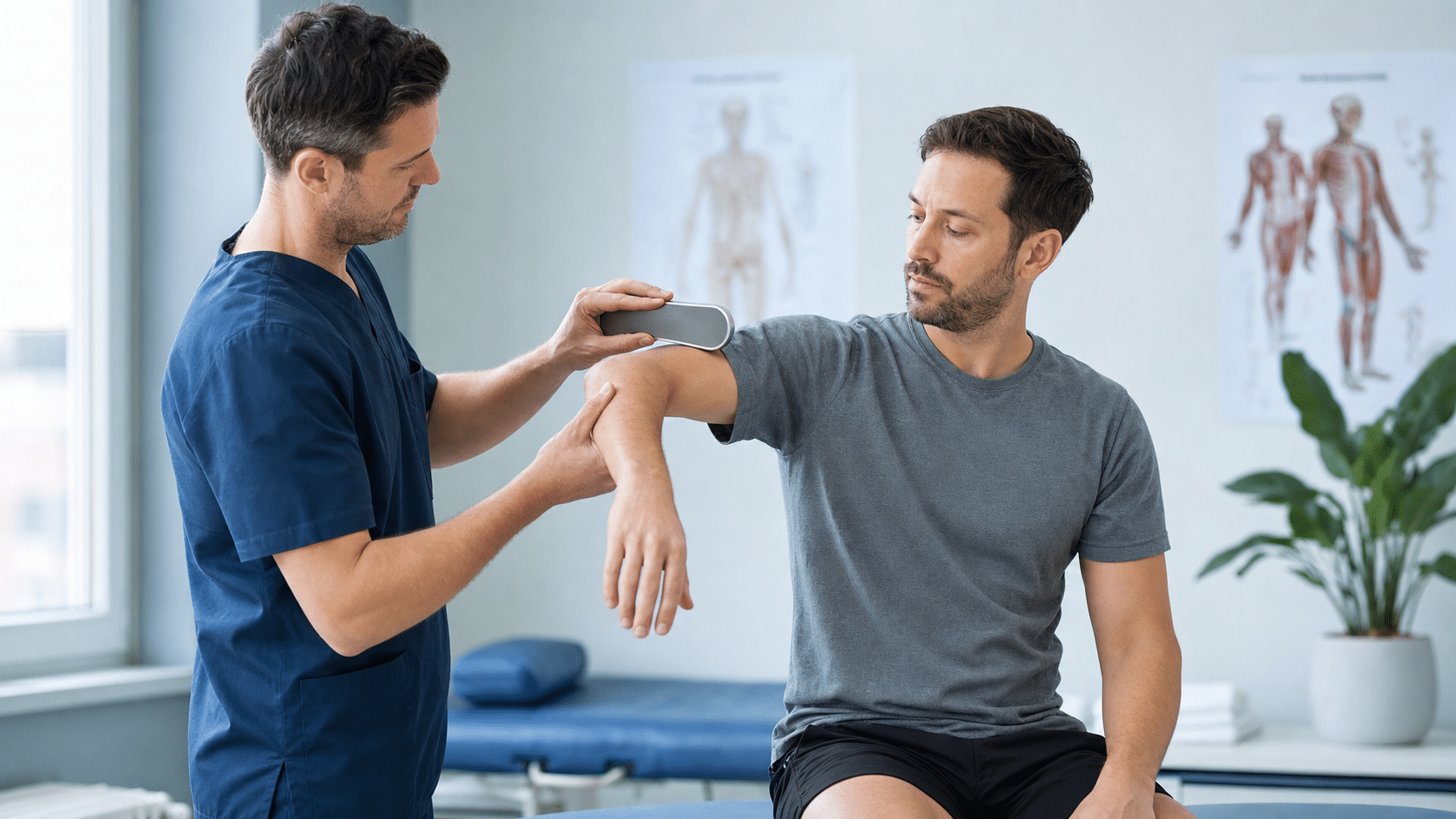
- May 27, 2026
Defensible Documentation: Why Objective Findings Hold Up When It Counts
How calibrated, objective measurements turn ordinary clinical notes into defensible documentation that holds up to insurance review, IMEs, and legal…
- May 26, 2026
You Can’t See the Whole Patient Picture Without a Functional Assessment
But here’s the catch: without a functional assessment, chiropractors only see part of the story. Structural findings alone may mask…

- May 26, 2026
How Much Will You Lose in Your Next Audit? The Silent Threat to Your Practice Revenue
Chiropractic audit documentation is the difference between getting paid and giving the money back.Imagine treating patients, submitting claims in good…

- May 07, 2026
Impairment Rating Guide: Accurate, Defensible Measurements
Accurate impairment ratings require more than clinical judgment — they depend on calibrated tools, reproducible protocols, and documentation built to…
