JTECH BLOG



Bringing Wellness to Work
 We spend a lot of time at work, doing the same thing day in and out, increasing the risk for repetitive injuries. Employee general well-being seems to be of increasing interest to employers. As a result, more and more employers are opting into wellness plans and offering incentives for those who participate. Some companies even go as far as to bring wellness to work and allow employees to participate during work time.
We spend a lot of time at work, doing the same thing day in and out, increasing the risk for repetitive injuries. Employee general well-being seems to be of increasing interest to employers. As a result, more and more employers are opting into wellness plans and offering incentives for those who participate. Some companies even go as far as to bring wellness to work and allow employees to participate during work time.
While it may seem counterintuitive to have employees doing anything but work during work hours, to these employers the benefits are clear.
According to a blog post by TodayinPT, loss of productivity due to strains and injuries has had a measurable impact on businesses, and even skeptical employees have noticed improvements from on-site therapy programs.
We have an onsite manufacturing plant [...] where a lot of our employees are male and wouldn’t make appointments to see a doctor until they were in a lot of pain,” Vissers said. “We want to help them to avoid long-term health problems by being proactive about their health, and realizing that pain isn’t an inevitable part of aging.”
While some of the manufacturing plant workers were unsure whether they actually could benefit from stretching [...] they were taught their roles at the company were as “industrial athletes” because of the lifting and physical labor required. Six months later, when their reach and other outcomes were measured again, employees saw the benefits of stretching. In the maintenance department pilot of 90 employees, only one strain was reported in a 10-month period, compared with 21 strains and sprains in the period before the pilot began.
Although a potential initial investment upfront, it seems wellness programs can offer a big return; employees receive preventative care and healthier employees tend to take fewer sick days. Identifying and reducing potential on the job injuries is a huge incentive as well and may encourage employers to implement pre-employment screenings or ergonomic evaluations once empoyees are on the job.
Some questions to consider:
As an employee, do you feel your employer provides adequate wellness incentives/resources?
As an employer, do you feel wellness programs are realistic and beneficial?
As a clinician, are you approached by employers to participate in similar programs or do you market to employers for these services?
Share this article:
Study Finds Physicians Do Not Consistently Follow Back Pain Guidelines
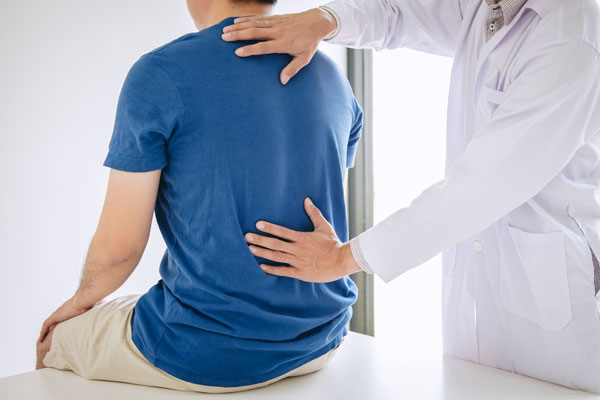 In a study published at Practical Pain Management, a survey of primary care physicians across 5 hospitals revealed that nonspecific back pain is inconsistently managed.
In a study published at Practical Pain Management, a survey of primary care physicians across 5 hospitals revealed that nonspecific back pain is inconsistently managed.
The study, conducted by students at Touro University, across an even spread of male and female physicians in New York City, posed a hypothetical question: how would you treat a patient presenting with acute, nonspecific back pain? Although some cases require specific treatment plans and specialist referrals, the results of the study show that nonspecific back pain may be handled differently by different physicians. This is done, according to the publication, despite the existence of several guidelines that offer courses of self-managed care and less "medicalized" options for initial treatment.
If a patient needs some pain relief, doctors should advise safe over-the-counter solutions, such as acetaminophen or a non-steroidal anti-inflammatory drug (NSAID), like aspirin or ibuprofen. If the pain persists, patients could try out some kind of secondary treatment, like spinal manipulation, acupuncture, yoga, or massage therapy, but these aren’t the first line of defense, noted the investigators.
The study also focused on some analysis of physician recommendations by gender, and found some interesting results:
- Male doctors were 10 times more likely to refer the patient to an orthopedist
- Male doctors were 2.5 times more likely to refer to a physiatrist, or physical therapist.
- Female doctors were more likely to prescribe medications (like muscle relaxants), thermal treatments, and spinal manipulation.
- Female doctors were also more likely to prescribe x-rays or CT scans.
The conversation around this subject is nuanced, and, as a commentator on the publication's website noted, "I'm sure there are lots of reasons [why], but I think it's a function of habit."
Read the Article JTECH Pain Evaluation Tools
Share this article:
Objective Findings: A Powerful Clinical Tool
As we start a new year, we often reflect on the progress we've made in the one coming to an end. Some of us may measure progress as trips to the gym, others in dollars earned, while others may keep track in more abstract measurements.
When it comes to the field of physical therapy, results are often measured by a patient's perceived changes. Am I stronger? Has the pain subsided? Can I perform functions I could not previously perform? But a patient's feelings are subjective, and can often be ambiguous, or influenced by emotions or perceptions. Objective findings become a powerful tool for a clinician in determining a patient's treatment plan and progress, while also serving as an easily understood and quantifiable value for the patient and referring parties.
In order to better understand the role that objective findings can play in a physical therapy practice, JTECH Medical sought out an expert. Jonathan Reynolds, PhD, PT, has been practicing physical therapy for over 25 years. During this time he has worked for hospitals and in private practice, worked on the design and development of two different software programs—JobSite 2 and the FCE module of the Northstar Occupational Medicine system—in conjunction with JTECH, designed his own lifting evaluation, taught continuing education seminars on Functional Capacity Evaluations and Job Site Analysis, created a tool—the TOLA System®—which allows patients to augment their therapy sessions at home, and developed research protocols for testing the functional capacity of dancers and musicians. Reynolds opened his clinic, Reynolds Rehab, with locations in Minneapolis and Eagan, MN. More recently, Reynolds Rehab partnered with Orthology. These clinics specialize in treating professional performing artists (dancers and musicians) alongside general orthopedic outpatient rehabilitation and industrial rehabilitation. With a background in research—having earned his PhD in Rehabilitation Science—Reynolds approaches his practice with objective data in mind, an approach that he thinks could benefit all practices.
"In our practice, we strive to provide evidence-based care," said Reynolds. "And while an evidence-based approach is often associated with research, it is also a powerful method with which to approach rehabilitation. If something can be proven effective, then it is evidence. Objective findings allow us to prove that a particular treatment plan has efficacy, and this evidence then qualifies what we do, while also helping us provide better and more productive care."
Including objective findings in a practice can help to build trust in relationships; and relationships are what Reynolds points to as a major contributor to his practices' ability to compete with larger clinics, which tend to refer within. Along with great treatment and care, Reynolds and his therapists ensure that they are constantly providing objective feedback to the referring parties, assuring them that the treatment is warranted and achieving results.
"Our success as a small practice is multi-faceted. Our therapists are well-trained and we have great communication. We are clear about the goals we want to meet and what outcomes we expect," said Reynolds. "Objective findings, like those we get with JTECH Medical's products, provide a platform for this critical communication. It allows us to build relationships with our patients, referring physicians, case managers, insurance companies, etc. And being able to track these outcomes objectively founds these relationships upon trust."
Orthology also uses manual therapy techniques as an integral part of rehabilitation. In the United States, most physical therapy is heavily exercise focused, but many people come to rehabilitation lacking the ability to immediately begin to exercise comfortably and effectively. To this end, Orthology helps patients arrive at a point in which they are comfortable with the exercise before they begin an exercise regimen. To help determine this point, the clinic incorporates objective findings alongside patient feedback.
"We can collect objective measurements when the patient first comes to our clinic, and then track their progress as we use manual therapy techniques," Reynolds said. "With the algometer and range of motion tests in particular, we are able to track the improvement and better decide when a patient will be able to be more comfortable and compliant with prescribed exercises. We then see strength gains with exercises performed at improved comfort levels."
At Orthology, each patient receives an objective evaluation before and after physical therapy, which allows the therapist to monitor the patient’s progress throughout treatment, and track outcomes. Depending on what outcomes they are tracking for a given patient, they will also perform a mini-discharge at the end of the treatment program, providing objective data that clearly points to a plateau in improvement, signaling the end of the physical therapy program.
"The objective findings are a critical component of our rehabilitation programs, but they can be a double edged sword," said Reynolds. "The person doing the evaluation needs to know what they are doing and how to interpret the data they receive. Education and ongoing practice is crucial to an evaluator's ability to accurately collect data, compare it from visit to visit, and interpret these results."
Reynolds stresses the need to use these systems that provide objective findings judiciously. At Reynolds' clinics, they make sure to use only the tools that are appropriate to a patient's injury and the targeted outcomes. In other words, even if they are able to completely test a patient's functional ability, their particular situation may not call for that, and it is important to use objective tools to validate the treatment plan that is required.
Incorporating objective findings into a practice can take on a variety of forms. Reynolds used JTECH's products when working on his doctoral dissertation, which focused on the shoulder mechanics and injuries in professional violin players. Since then, he has used the tools in other research projects aimed at grip strength as well as further research into shoulder mechanics. He also incorporates objective findings in other more traditional ways, such as for Functional Capacity Evaluations (FCEs), as well as work hardening, ergonomic, and job site evaluations.
"From an FCE standpoint, an evaluator's most powerful tools are his or her eyes. A system that you can rely upon to accurately collect objective data about the performance allows you to keep your focus entirely on the patient, observing their behavior and effort," said Reynolds. "You can also take the equipment to a job site and tell the employers the relative risk of workplace activities. Using the JobSite 2 software tools, such as the NIOSH Lifting Equation tool, or the Cumulative Trauma Disorder risk assessment tool, I can pinpoint the issue. Is it repetition? Too much weight? Is the worker reaching too high or too low? With the objective findings, you can point out which changes need to be made right there on the spot."
These skills require proper training and constant practice. Reynolds first received his FCE and ergonomic training through seminars, and he continues to use these skills every day, including teaching them to other practitioners. His therapists, too, receive training, are constantly practicing, and receive periodic in-house training sessions to ensure that they are able to use these tools to obtain meaningful data.
"I could teach my sixteen-year-old son to use the equipment to collect all of the data, but he wouldn’t know what he was doing," said Reynolds. "He could make the evaluation look and feel legitimate, but the data would be meaningless. It is imperative that the evaluator be skilled and properly trained in obtaining meaningful objective data, and that this education remains an ongoing process."
Learn More About:
Algometry Grip Strength Range of Motion Muscle Strength JobSite 2 Software
Share this article:
Occupational Therapy May Help Fortify Aging Populations
As populations age around the world, the difficult task of caring for conditions like dementia is being addressed by occupational therapists. The personally-targeted methods employed by OTs might help those who suffer dementia cope, or may even delay the onset, according to a report.
In Singapore, where the elderly population is rapidly growing, adding 300 to 400 more occupational therapists to a preventive care program could "significantly" reduce the negative effects of dementia, as opposed to a strictly "assisted living" approach that may not help with overall health and function in the long term.
"Getting dementia patients to carry on doing things helps them maintain their ability to function ... [and] having a maid do everything for them could result in a more rapid decline."
Preventive care services that focus on functional ability are seeing more widespread adoption all the time. What other new programs have you heard about or participated in? Let us know!
Share this article:
The Impairment Rating - An Objective Indicator of Functional Ability
Serious injuries can happen anytime and anywhere. On the motorway, while performing work duties, or even at home. If the injury sustained is serious, these accidents may lead to legal or insurance claims. However, getting the person who was injured and the insurance company to agree on the magnitude of the injury is near impossible.
When these serious accident or injuries happen, there are often more questions than answers. How bad is the injury? How long will it take to heal? How will this affect the ability to work? Will this lead to a permanent disability? Is there a way to qualify for financial help?
Fortunately, the answers to these questions can come through working with a qualified medical professional. One such type of test, an independent medical exam (IME), allows the medical professional to evaluate what happened and identifies injury. Another type an evaluator might perform is called a Functional Capacity Evaluation (FCE). In this physical examination, the injured person will perform different tasks to test their ability to perform normal daily activities. This allows the medical professional to evaluate the injured person’s capability to perform work related tasks. Both of these assessments evaluate whether or not the patient has an impairment – a problem that affects the body’s function and makes the patient unable to use their body as they did before the injury. These tests might include evaluation of range of motion, strength, ability to balance, lifting, and more.
There are a wide range of impairment types. Some might not be as concerning as others. One important distinction is whether or not the impairment is temporary or permanent. Impairments classified as temporary do not have the same bearing as a permanent classification. For those who have a permanent impairment, they are subject to receive an impairment rating.
An impairment rating quantifies the injury and scales the impairment’s severity. This rating is determined by a medical professional in an Impairment Rating Evaluation (IRE) and takes place after the patient has reached their maximum medical improvement. The impairment is quantified as a percentage between 0 and 100. This rating acts as one of the most important pieces of information in a benefit claim to keep receiving financial aid. The results of the IRE appointment will help the injured person’s attorneys determine how long a person will receive benefits, the amount of benefits they will receive, and whether they are expected to be able to return to work. It carries immense weight in the determination of the extent of financial aid the injured may have entitlement to.
The key personnel in these cases is the medical professional. Disagreements often arise between an injured person and an employer or insurance agent. Patients generally want the most compensation they can receive while employers or insurance agents may downplay the injury to avoid paying out extended benefits. While most people are honest about injuries, insurance fraud and mislabeling are concerning. Medical professionals act as the unbiased evaluator on the extent of the injury. Again, the amount of compensation the patient receives depends highly on the impairment rating.
The biggest help in an effective impairment evaluation is a medical professional’s own expertise and experience. The next biggest help is proper and professional evaluation tools. The right tools aid a medical professional in turning subjective data concerning a patient’s injury into objective and measurable information– data that now proves use in helping clients receive the proper amount of compensation. JTECH Medical provides several robust computerized functional testing system options. JTECH’s Occupational Medicine Testing Systems offer all of the essential Functional Capacity Evaluation (FCE) testing equipment to objectively assess, document, and track a subject’s physical abilities. The same systems also contain all the instruments to perform an effective IME evaluation. After using the instruments, our advanced software easily generates narrative and graphical reports showing a summary, details, and history of each test. These reports will then help you generate impairment ratings based on the American Medical Association (AMA) guides. Your personal expertise paired with JTECH Medical equipment smooths out what can be very complex evaluations.
Together, we can elevate the patient’s path toward recovery and wellness.
Share this article:

